GP practices across England are increasingly questioning whether they can continue delivering the annual flu vaccination programme, as many believe it is no longer financially sustainable. The British Medical Association (BMA) has formally raised concerns with Professor Chris Whitty, warning that stagnant funding and rising operational costs are placing serious pressure on general practices.
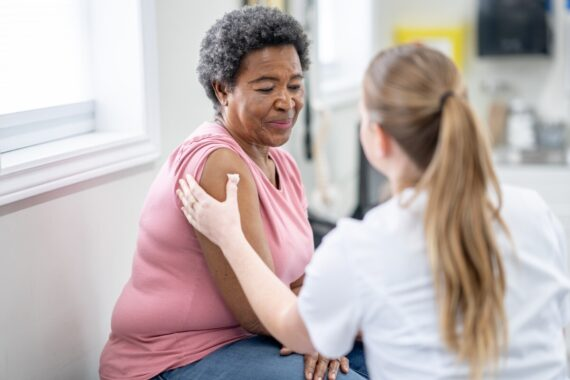
According to the BMA’s GP Committee, payments for routine immunisation services have not been significantly increased since 2019/20, despite inflation and rising staffing expenses. Running flu clinics requires additional clinical time, administrative support, vaccine storage, and temporary staff, all of which have become more expensive.
However, funding levels have remained largely unchanged, making participation in the programme increasingly financially unviable for many practices. Some GP surgeries are reportedly considering not signing up for next year’s flu campaign or delaying vaccine orders.
Department of Health and Social Care

The Department of Health and Social Care (DHSC) is a United Kingdom government department responsible for overseeing the country’s health and adult social care systems. It sets national policy, allocates funding, and ensures that services such as the National Health Service (NHS) and social care providers deliver safe, effective, and efficient care.
Key facts
- Formed: 1988 (as the Department of Health; renamed DHSC in 2018)
- Headquarters: 39 Victoria Street, London
- Current Secretary of State: Victoria Atkins (as of 2024)
- Main agencies: NHS England, UK Health Security Agency, Medicines and Healthcare products Regulatory Agency
- Jurisdiction: England (healthcare and social care policy)
Mandate and functions
The DHSC leads government efforts to improve the health and wellbeing of people in England. Its responsibilities include funding and strategic oversight of the NHS, setting standards for public health, and guiding social care policy. It also handles emergency preparedness, medical research funding, and coordination with devolved governments on UK-wide health issues.
Structure and agencies

The department operates through several arm’s-length bodies and executive agencies. NHS England manages day-to-day healthcare delivery; the UK Health Security Agency addresses infectious disease and biosecurity; and the Medicines and Healthcare products Regulatory Agency ensures the safety of medicines and devices.
These agencies implement DHSC policy while maintaining operational independence.
Role in public health and social care
The DHSC develops national strategies on prevention, health inequalities, and adult social care reform. It oversees workforce planning for health professionals and regulates social care providers in England. During crises such as the COVID-19 pandemic, the department coordinated the national response, procurement, and vaccination efforts.
Current priorities
Current priorities include reducing NHS waiting times, integrating health and social care services, supporting mental health initiatives, and modernizing digital health infrastructure. The DHSC also focuses on long-term sustainability of care funding and addressing disparities in health outcomes across regions.
NHS England has announced that the item of service fee for adult flu vaccinations will be £10.06 in 2026/27, while practices can claim £8.70 per vaccine administered during the main campaign period. At the same time, the additional £10 payment for vaccinating housebound Covid-19 patients has been removed, raising further concerns among GPs. Many argue that current payments do not reflect the true cost of delivering vaccinations, especially to vulnerable patients requiring home visits.
Local medical committees warn that removing the housebound vaccination fee could make outreach services financially unsustainable, potentially impacting elderly, high-risk, and housebound patients. GP leaders stress that continued underfunding may force practices to make difficult financial decisions, including reducing staff or limiting additional patient services.
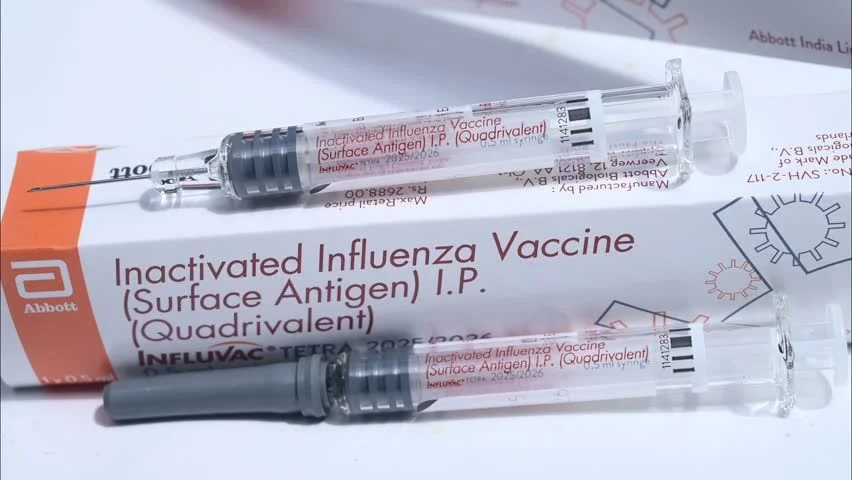
In response, the Department of Health and Social Care has highlighted an additional £1.1 billion investment in general practice, bringing total GP contract spending to £13.4 billion in 2025/26. The government also plans to recruit 2,000 additional GPs and has reaffirmed its commitment to maintaining vaccine access. However, GP representatives argue that vaccination payments have fallen significantly behind inflation in real terms.
The wider public health impact is significant. In his annual infectious disease report, Professor Chris Whitty emphasised the need for a more systematic approach to infection prevention, particularly among older populations at higher risk of severe illness. If more GP practices withdraw from the flu programme, vaccination uptake could decline, increasing NHS winter pressures and widening health inequalities.
FAQs
#NHS #FluVaccine #GPFundingCrisis #Carrerbook #Anslation #HealthcareNews #PublicHealth #FluJab #NHSFunding #UKHealthcare #VaccinationDrive
